
Breaking down the microbiology world one bite at a time
Fermented food fighting for us – Part II
In our previous article, “Fermented food fighting for us part I”, we explored the difference and summarized a few mechanisms in which fermented foods, bacteriophages, and bioactive compounds vacillate by hurting or helping the overall health of the host. Now, in Part II, we will explore a series of review articles that discuss the potential health benefits of fermented foods, and how the lactic acid bacteria (LAB) and their metabolites protect the host from respiratory tract infections (RTI).
In Part I, Bousquet and his colleagues suggested that geographic regions, in which people consumed fermented foods on a regular basis (specifically fermented cabbage), had lower COVID-19 mortality rates. The authors attributed the lower mortality rate to that of fermented cabbage consumption, which is rich in sulforaphane (sulfur-rich compound)and LABs. The combination of sulforaphane and LAB was thought to not only lower insulin resistance, an important comorbidity affecting survival outcomes in infected COVID-19 patients, but also to influence the outcome of the infection itself. The authors hypothesize both sulforaphane and LABs activate NRF2, an important enzyme that inhibits the oxidative stress pathway- which is thought to be triggered by the virus itself.
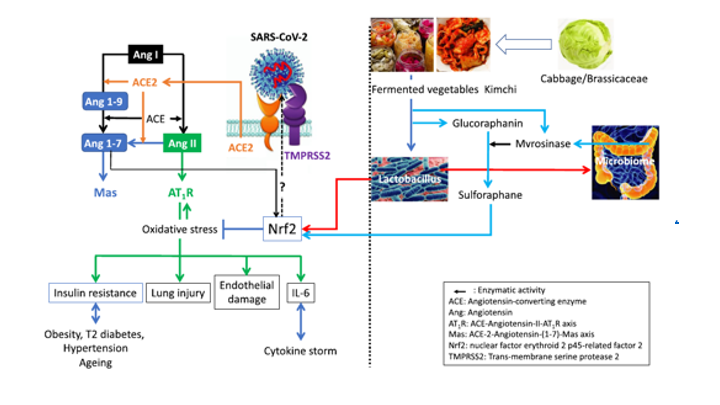
Note: We encourage you to approach articles about COVID-19 with a healthy dose of skepticism. Generally, journals stress that the urgency of the pandemic can affect the quality of the publications. The authors themselves admit the shortcomings of their analysis, but, considering the pressures of understanding and mitigating the detrimental effects of the virus, they felt compelled to share their observations.
Despite the author’s erratically compiled results from an assortment of mortality metrics and other limitations associated with a hurried study, it is not an inconceivable concept. Fermented foods, which are rich in probiotics and other beneficial metabolites, could undercut some of the most dangerous symptoms of RTI, including those of COVID-19.
A SUMMARY OF RESPIRATORY TRACT INFECTIONS
Respiratory tract infections are typically viral in nature and range from the common cold to the deadly influenza that plagued the globe in 1918. The more benign RTIs occur in the upper respiratory tract, where infected individuals would suffer from sinus pressure, runny noses, and sore throats. Infections turn menacing, if they take root deep in branches of the lower respiratory tract, where they can wreck a long term damage.
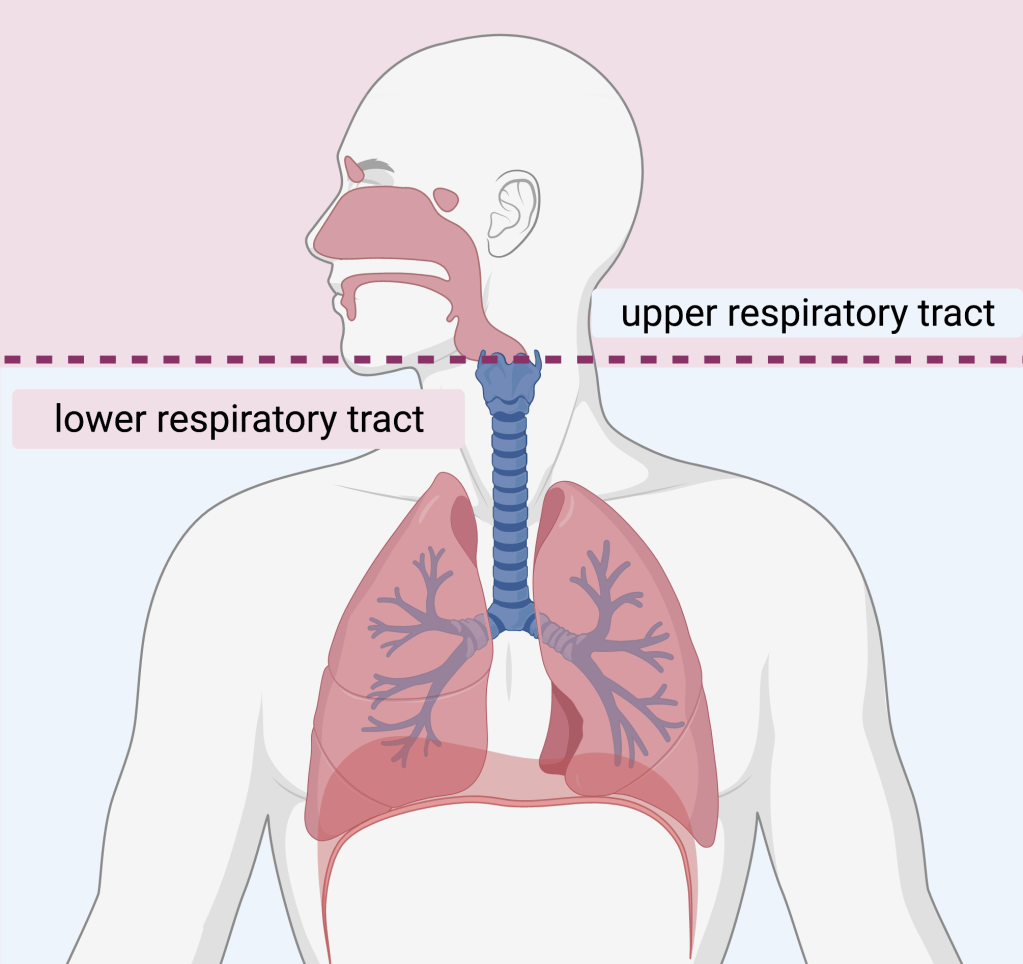
More serious and deadly viral RTIs trigger a “cytokine storm.” This causes an imbalance of innate and adaptive immunity, leading to a hyper-responsiveness that makes viral infections lethal. For example, COVID-19 is famous for causing cytokine storms, particularly in older and immunocompromised individuals, whose immune systems recognize too little, too late. This results in a melee of immune modulators frantically attacking the high concentration of the respiratory virus.
A fight like this results in a serious weight loss, long term damage to the lungs, which dramatically reduces pulmonary function, and an increased risk of secondary infections. In fact, it could still be a second wave of the same infection. Increased viral titers in the pulmonary serum could make it difficult to effectively clear out pro-inflammatory actors over a longer period.
RESPIRATORY TRACT INFECTIONS – A MULTISYSTEMIC ORIGIN STORY
The predisposition of developing a secondary infection is, in fact, linked to the gastrointestinal (GI) tract and the gut microbiome itself. The magnitude of secondary effects of a respiratory infection are also indicative of the complex interactions between different organ systems.In fact, it is widely believed the GI tract and its microbiome plays a role in mitigating the host’s susceptibility to RTIs. A healthy gastrointestinal system with an army of commensal microorganisms can prime the host for any hidden danger. This happens with the help of the gut associated lymphoid tissue (GALT), which represents a series of localized immune cells and structures that search and destroy pathogens or tolerate commensal microorganisms and food particles that pass through the system. Whenever GALT is impaired, opportunistic pathogens, both viral and bacterial, easily slip through permeable intestines to terrorize other organ systems.

Mahooti et al. conducted a systematic review of interventional studies in both human and murine models, and concluded that lactic acid bacteria in fermented foods can influence the prognosis of respiratory tract viruses via three mechanisms:
1. Directly interact with the epithelial cells which could lead to a cytokine cascade. Probiotics can activate toll-like receptor proteins and other pattern recognition proteins can recognize pathogen-associated molecular patterns in viruses.
2. Dendritic cells that serve as scouts along the gastrointestinal tract, sampling a diverse array of bacteria, including lactic acid bacteria found in fermented foods and probiotic products to keep the immune system up to date.
3. Direct interaction with GALT cells, like macrophages and M-cells, leads to increased mucosal secretion and triggers the adaptive immune response.
Mahooti also highlighted that the beneficial effects of these probiotic strains were more apparent, when probiotic organisms were in fermented foods or in a form of capsules ingested and processed in the gastrointestinal tract, rather than injected directly.
Darbandi and colleagues’ collection of articles was different because it excluded animal models and only allowed peer-reviewed interventional clinical trials, which included the confirmation of the overall benefits of probiotics for humans. Though lacking in detailed mechanism of action like in the review by Mahooti et al., Darbandi et al.’s compilation suggested that the consumption of probiotics and fermented foods leads to an efficient immune response (without triggering a cytokine storm) and increased gut microbiome diversity, which reduced the probability of secondary RTIs. They also reported studies, in which probiotics were combined with vaccinations, leading to greater vaccine effectiveness. Additionally, studies observed that a continual administration of probiotics reduced the likelihood of developing RTIs during the flu season (although this does not work in immunocompromised individuals or elderly adults suffering from immunosenescence).
But wait, many of these studies are done with single strains of probiotics that come in a capsule form? Why bother eating fermented food?
Firstly, not everyone responds to probiotics the same way. Many studies have identified strains that are successful, but are population-specific. For example, Darbandi’s colleagues highlighted a study, where the composition of the gastrointestinal microbiome was linked to a strain’s ability to provide the sought-after benefits. Though certain microbiome profiles are less likely to respond to the probiotic treatment, studies suggest that a consistent consumption of a variety of probiotic-rich fermented foods could help to shift the GI microbiome profile to improve the overall health and lower susceptibility to RTIs. Authors Ögel & Özturk, take it one step further.
In part I, we explored the possible risks of ingesting unregulated fermented food products. Ögel & Özturk suggest that consuming fermented foods from unidentified strains is well worth the risk. Even mixing a variety of them into a single dish will increase the likelihood of ingesting an efficacious or series of probiotic strains.
Note: MicroBites would like to warn you that ingesting probiotic foods with unidentified strains is not always safe. Adverse events related to the gastrointestinal tract still can occur, even with strains that were tested for safety.
Back to why eating fermented foods has additional benefits. The way in which probiotics are introduced appear to play an important role in their efficacy. In one study, respiratory tract infected mice were provided with one of two types of LAB medication. The first is a tablet that dissolves under the tongue (sublingual medication) and another a capsule of probiotics that doesn’t release the LABs until further along the GI tract. The researchers monitored the evolution of the RTI symptoms, such as systemic inflammation markers and viral loads within pulmonary fluid. They found that mice provided with the sublingual were significantly improved than mice who were given capsules. In the review article written by Ögel & Özturk, it was suggested that when probiotics (in the form of fermented foods) enter the body , chewing and savoring foods allow LAB to diffuse with the oral microbiome. The LABs in the oral microbiome and their proximity to the pharynx allow the produced metabolites to enter the upper respiratory tract.
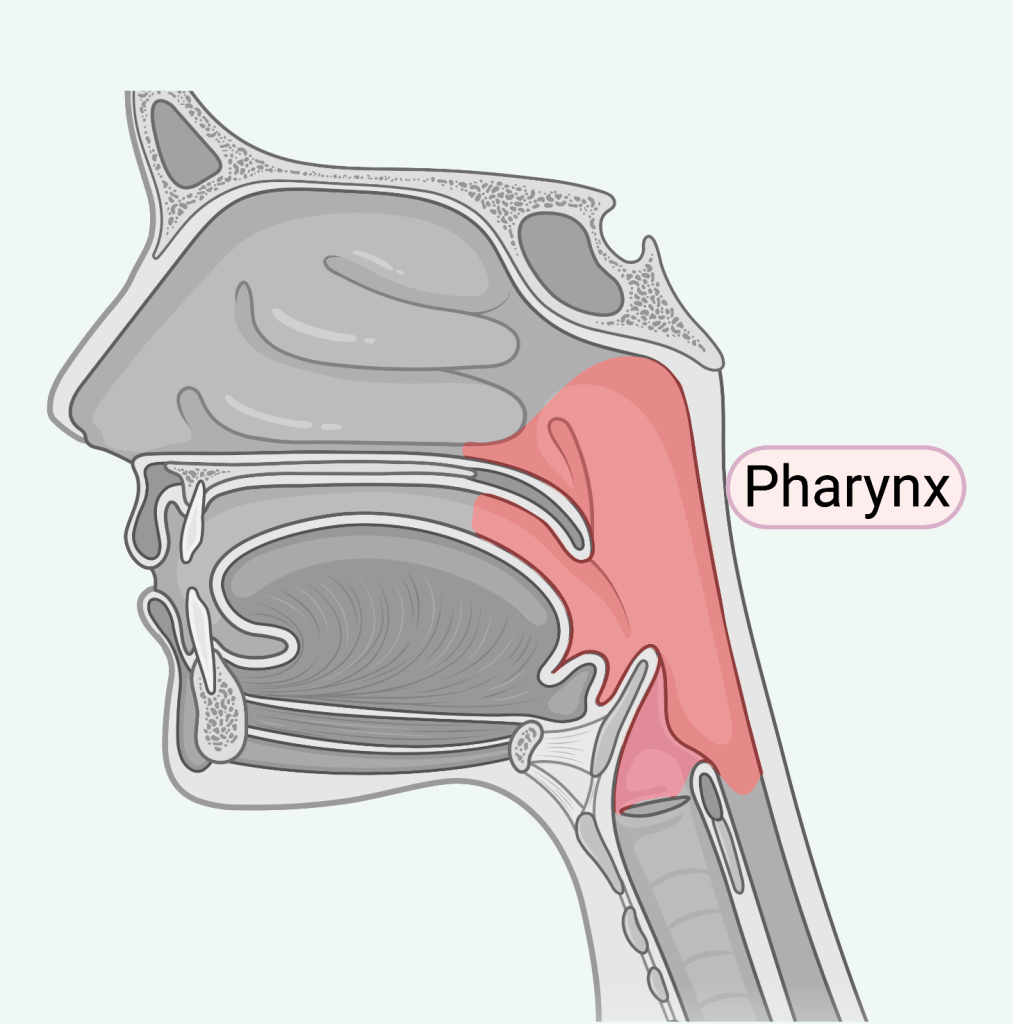
Another possible prophylactic benefit of fermented foods is the presence of metabolites derived from fermented foods. Recall that Bousquet and colleagues theorized that fermented cabbage contains a combination of sulforaphane and LABs that trigger an anti-oxidative response. Some examples of other bioactive compounds metabolites within fermented foods are polyphenols, bioactive peptides, conjugated linoleic acid, gamma aminobutyric acid, and vitamins. These compounds are present in the food products themselves, and are going to be either processed by LABs, or be further metabolized by gut microorganisms. This group of metabolites directly or indirectly interacts with the immune system, although the exact mechanism of action remains undetermined.
In conclusion, the benefits of consuming fermented foods appear to not be limited to the gastrointestinal tract. Though the research suggests that fermented foods decrease the likelihood of developing RTI and reduce symptoms of existing RTI, the exact mechanism is still unclear. More research is needed to validate whether a diet rich in fermented foods decreases the mortality rate in COVID-19 infected individuals. However, considering the current state of the pandemic, it wouldn’t hurt to adapt and incorporate fermented foods into one’s diet (in addition to taking peer-reviewed and approved measures by trusted scientific institutions, of course).
Links to the original posts:
Featured image: Created by author with BioRender.com



































































































