
Breaking down the microbiology world one bite at a time
What If Vaccines Didn’t Need Needles?
Viruses commonly initiate infection at mucosal surfaces such as the respiratory tract. To protect these vulnerable interfaces, the immune system has evolved specialized barrier defenses referred to as mucosal immunity. Immune cells and locally produced antibodies at these sites can limit viral spread before viruses reach deeper tissues. However, these immune defenses are not always sufficient to prevent severe illness, highlighting the importance of additional preventive measures such as vaccination. Vaccines expose the immune system to harmless pathogen components (e.g., viral proteins) that are sensed by immune cells. This priming will establish long-lasting protective responses and enable faster and more effective reactions upon subsequent exposure.
Despite vaccination-induced protection, robust mucosal immunity remains difficult to achieve. The predominance of injection-based vaccines, which primarily stimulate systemic rather than mucosal immunity, has prompted the need for needle-free delivery strategies to better target immune defenses at viral entry sites.
A recent study in Nature Biomedical Engineering reported an unconventional strategy using dental floss to deliver vaccines directly to the gums.
The Oral Cavity: Accessible but Restrictive
The oral cavity is an attractive site for vaccine delivery thanks to its accessibility and near-neutral pH, which can help preserve vaccine molecules. Previous efforts have focused on administering vaccines under the tongue or along the cheek. However, vaccine delivery at these sites has been limited due to poor tissue permeability.
The researchers instead focused on a less studied region of the mouth: the gingival sulcus, the narrow space between the teeth and gums. At the base of this space lies the junctional epithelium, a thin tissue that anchors the gums to the teeth.
Unlike most oral tissues, the junctional epithelium is naturally permeable and enriched with diverse immune cells, supporting continuous immune surveillance at the gum–tooth interface. Because this region is constantly exposed to dense microbial communities, its unique immune composition makes it a potential site for initiating protective responses.
The question is, how could vaccine material be delivered to this specific site to elicit a robust immune response?
Using Floss to Target the Gingival Sulcus in Mice
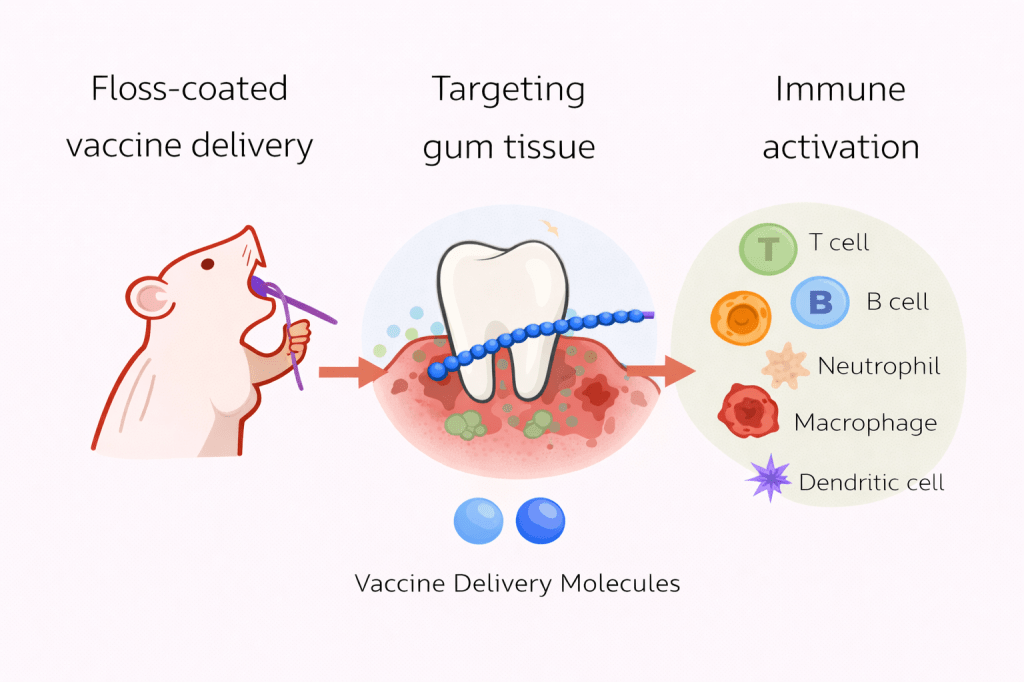
Liquid vaccines placed in the mouth are quickly removed by saliva, swallowing, or food intake. Dental floss naturally passes through the gingival sulcus, allowing the coated material to come into direct contact with the junctional epithelium during application. After floss removal, a substantial portion of the material remains deposited within the tissue, see also the schematic overview below.
A key question was whether delivering vaccines through the gums could generate mucosal immune responses beyond the oral cavity. To answer this, the researchers tested the dental floss vaccine in mice. In vaccinated mice, antibodies were detected not only in the bloodstream but also at multiple mucosal sites, including the lungs, nasal passages, saliva, and gastrointestinal tract. Immune responses were further observed in lymph nodes and the spleen, and antibody-producing cells were detected in the bone marrow, suggesting the development of long-lived immune memory.
To determine whether the floss-based vaccine provided protection against viral infection, the researchers challenged the vaccinated mice with a lethal dose of live influenza virus. Mice that received three doses of the floss-based vaccine survived, whereas unvaccinated mice did not. Protection was comparable to intranasal vaccination and stronger than vaccines delivered under the tongue. Furthermore, older mice were also protected, indicating that the response was not limited to young animals.
Assessing Feasibility in Humans
To assess whether this delivery approach could be translated to humans, the researchers conducted a small feasibility study using floss picks coated with a fluorescent dye. Healthy adult volunteers flossed as usual, and delivery to the gingival sulcus was quantified. On average, approximately 60% of the dye reached the target tissue. While immune responses in these individuals were not evaluated, the findings demonstrated that floss can reliably deliver material to the junctional epithelium in human mouths. Notably, most participants also reported a willingness to receive vaccines using this approach.
Implications of the Findings
This study identifies the gingival sulcus as an underappreciated site for vaccine delivery and shows that dental floss can precisely target this immune-active tissue in mice. While floss-based vaccination has not yet been evaluated in human clinical trials, factors such as gum health, oral inflammation, dental variability, and long-term safety will require further investigation.
The work presents a complementary strategy for mucosal vaccination by taking advantage of a tissue naturally involved in immune surveillance. These findings provide insight into how anatomical context influences immune responses at barrier surfaces. Together, the results not only advance our understanding of mucosal vaccination but may reveal new therapeutic possibilities hidden within overlooked anatomical sites.
Link to the original post: Ingrole, S. J. Rohan et al. “Floss-based vaccination targets the gingival sulcus for mucosal and systemic immunization” Nat Biomed Eng.. 2025 Jul 22. Doi: 10.1038/s41551-025-01451-3.
Featured image: The image is generated with Open AI















